You can’t will yourself calm — but you can signal your nervous system that safety has arrived. The vagus nerve is how that signal travels.

Most of us know what it feels like when the stress response fires — the chest tightening, the narrowing of focus, the low hum of readiness that doesn’t quite switch off at the end of the day. What fewer of us know is that there’s a dedicated neural pathway whose entire job is to apply the brakes. It’s called the vagus nerve, and learning to activate it is one of the most practical things you can do for your own wellbeing.
The longest nerve you’ve never thought about
The vagus nerve runs from the brain stem all the way down through the neck, chest, and into the abdomen — touching the heart, lungs, and gut along the way. It is the primary conduit of the parasympathetic nervous system, carrying signals in both directions: downward from brain to organ, and upward from body to brain. That bidirectionality matters. It means the nerve doesn’t just receive instructions from above — it actively reports on the state of the body, influencing mood, emotional regulation, digestion, immune response, and heart rate in the process.
The measure of how well it’s doing its job is called vagal tone. High vagal tone shows up in your HRV data as flexible, responsive variation between heartbeats — a sign that your autonomic nervous system can shift gears smoothly. Low vagal tone tends to correlate with heightened stress reactivity, difficulty recovering from pressure, and over time, an increased vulnerability to anxiety and depression. Vagal tone is not fixed. It is trainable.
“Many of the activities we associate with calmness — deep breathing, meditation, even the experience of awe — work in part by increasing vagus nerve activity.” — Cedars-Sinai
How guided meditation activates the vagal brake
When you slow your breathing during a guided session, you’re doing something physiologically precise. Research published in PMC identifies slow, extended exhalation as the primary mechanism of what scientists call respiratory vagal nerve stimulation — a direct, rhythmic activation of the vagus through breath pacing. The exhale is the key moment: it’s when the heart rate naturally drops and the parasympathetic system asserts itself. A longer exhale means a longer window of vagal engagement.
Guided body scans add a second pathway. By systematically directing attention through the body without judgment or urgency, they reduce activity in the brain’s default mode network — the region associated with rumination and self-referential threat monitoring — while signalling to the motor system that no action is needed. The body interprets stillness and guided attention as environmental safety. The vagal brake engages.
A 2025 randomised controlled trial from University College London confirmed this is not just metaphor. Researchers found that combining vagus nerve activation with compassion meditation produced significantly greater gains in mindfulness and self-compassion than either approach alone — suggesting the nerve doesn’t just carry calm, it amplifies the training effect of the practice itself.
Three tools your breath already owns
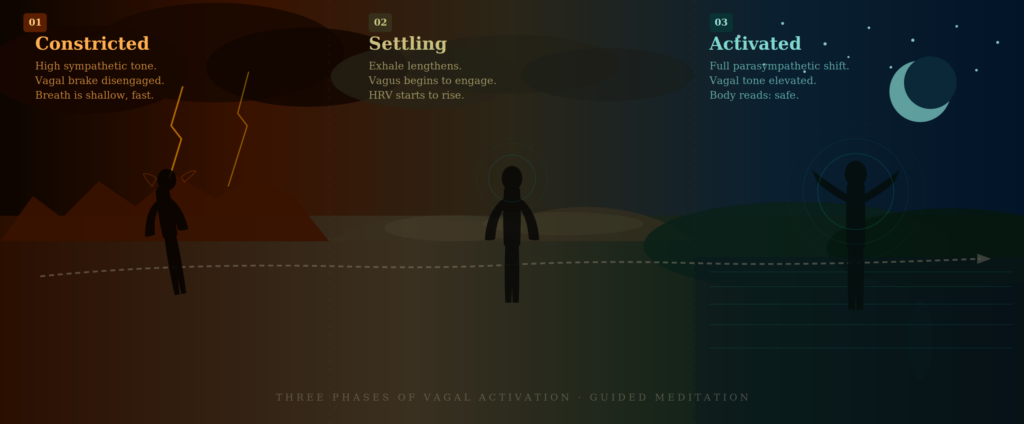
one of these require equipment, a dedicated hour, or belief that they’re working. The vagus nerve responds to input, not intention. You give it the right conditions — slowed breath, body attention, the absence of perceived threat — and it does the rest. Over time, and with repeated practice, the range of your vagal tone expands. The stress response still fires when it needs to. It just stops running the show.

